In the last few weeks, there has been an uptick in the discussion of rising Medicare hospice costs and the role of fraud in the phenomena.
The headlines feel like a rush to judgment and it worries me. I don't think that most people understand the first thing about hospice and in the current budget cutting environment, I worry that we will make a mistake that will deprive people at the end of their lives of valuable services and that we could even unintentionally increase total health care costs while trying to lower them.
So today, a primer on hospice – the U.S. version – and in the next post I will provide some alternative analysis. For this background, I draw on the National Center for Health Statistics and the Medicare Payment Advisory Committee. First, while most people think of hospice as a place you go, in over 90% of cases it is not. The dying person doesn't go somewhere, but rather gets a set of services delivered at home (55% of cases), in a nursing home (26%), or even in a hospital (10%). As one might guess (hope?), the vast majority of hospice clients are older adults – over 80% are over 65 and therefore Medicare is the dominant payer. Given its roots in cancer treatment, it's no surprise either that 44% of patients on average still have cancer as their primary diagnosis/terminal condition.
Under Medicare regulations, beneficiaries are eligible for hospice if they agree to forego "curative" treatment and if a physician will certify that the patient has six months or less to live under the normal course of his or her disease. In return for providing comprehensive supportive and palliative care, from counseling to medications to even surgical interventions designed to reduce pain and suffering, the hospice agency gets paid a daily case rate of $143 with a range of modifications covering the intensity of services in a day and geographical modifications adjusting for wage rates. Because death is hard to predict, hospice patients can be recertified as appropriate for the benefit after the initial 6-month period. The government has made considerable efforts to reassure everyone concerned that good faith "excess survival" will not be held against anyone.
Unfortunately, there is little information available about the quality of care in hospice. But one major marker, the median number of days people get care before discharge (largely due to their death), is only 16. (So . . . 50% of hospice participants receive less than 16 days!) Only 37% of those receiving hospice services in 2007 got at least 30 days of service, considered the minimum amount of time to fully deploy the model and support people who are dying and their families. The other 63% are getting help that is surely better than nothing, better than staying at the hospital, better than the minimal pain control that is all too common, but not exactly what one would want.
Nevertheless, the attention has all been focusing on overuse of hospice and rising costs. What gives? First off, costs of hospice overall have been rising because more people are using it. This is a good kind of cost increase. In 2008 almost 40% of Medicare beneficiaries who died got hospice care as opposed to 23% in 2000. This "increase" in hospice costs may even be cost saving depending on what kind of health care services might have been used instead (and how they were paid for).
However, the second cause of cost increases is more ambiguous. While the length of stay "in hospice" remains too short for most, there has been growth in the small number of people receiving hospice services for very long periods (around a year), particularly in for-profit agencies for conditions like Alzheimer's disease, which typically receive less intensive care. For example, the percent of patients receiving care for more than a year is 4.1 for all providers (death is hard to predict). But the percent of for-profit cases over a yearlong period is 6.9 as compared to 2.8 from nonprofit agencies. Not big numbers, but troubling at $143 a day.
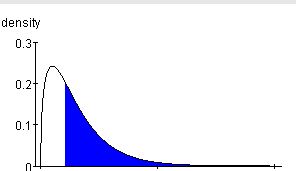 I imaging that the frequency distribution of length of stay looks something like this:
I imaging that the frequency distribution of length of stay looks something like this:
The median (16) is the boundary of the un-shaded and shaded sections and the long skewed tail to the right represents the fact that there are very long-term cases, but they are very few. The question of long-stay cases boils down to a small bump out at the thin tip of the tail.
This discussion has been going on for some time. Last year's MedPACreport included a discussion of suspicious pattern of service utilization and billing. And in February 2011, a long-time Hartford grantee, Ed Marcantonio, MD, was among a team publishing an analysis: Association of Hospice Agency Profit Status With Patient Diagnosis, Location of Care, and Length of Stay in JAMA . Their work strongly suggests that by virtue of taking more non-cancer patients with lower intensity needs and longer lengths of stay, for-profit hospices are gaming the system in an inappropriate way.
At the time, I made some comments on other blogs about the issue here but I think the topic deserves still more discussion . . . stay tuned for Part II.

